
Crashed motorcycle lying on its side on asphalt road with skid marks and scratches on the pavement surface
Road Rash from Motorcycle Accidents – Severity, Treatment, Recovery Guide
Asphalt doesn't forgive. When a rider separates from their bike at speed, skin meets pavement in a friction battle that skin always loses. Road rash—the deceptively casual term for traumatic skin abrasion—accounts for roughly 70% of all motorcycle accident injuries. Unlike broken bones that announce themselves with obvious deformity, road rash damage isn't always apparent until you peel back clothing or adrenaline fades.
Understanding what happened to your skin, how deep the damage goes, and which treatment decisions matter most can mean the difference between clean healing in weeks versus infection, scarring, and months of complications.
What Happens to Your Skin During a Motorcycle Crash
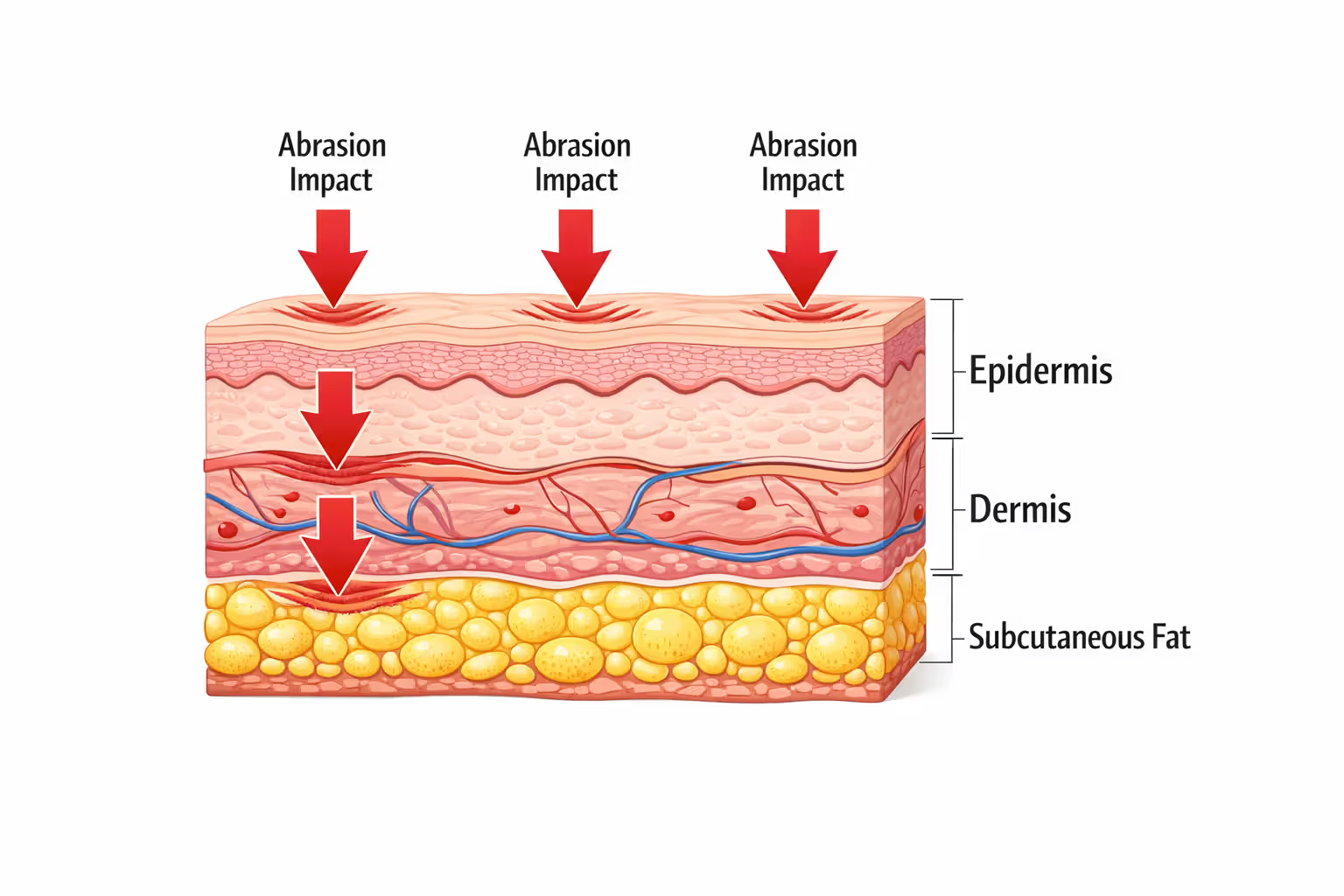
Your skin has three main layers: the epidermis (outer protective barrier), dermis (containing blood vessels, nerves, and hair follicles), and subcutaneous tissue (fat and connective tissue). During a slide or tumble, friction generates enough heat to literally burn away these layers while simultaneously grinding debris—gravel, dirt, glass, asphalt particles—deep into the wound.
Motorcyclists face particular vulnerability because even armored gear has limits. A jacket rides up during impact. Gloves tear at the palm. Jeans offer practically zero abrasion resistance above 30 mph. The resulting motorcycle accident skin injuries guide reveals a predictable pattern: elbows, shoulders, hips, and knees take the worst damage because they're both impact points and pivot areas during a slide.
The mechanical process combines three destructive forces. First, the initial impact tears the epidermis. Second, continued friction as you slide generates temperatures exceeding 200°F—enough to cause thermal burns alongside the abrasion. Third, the grinding action embeds foreign material that your body will later try to wall off or expel, creating infection risk and potential tattooing if not properly removed.
Speed matters exponentially. At 20 mph, you might escape with superficial scraping. At 45 mph, expect dermis involvement. Above 60 mph, you're looking at potential full-thickness injuries that expose fat, muscle, or bone.
Author: Ryan Whitlock;
Source: spy-delhi.com
The Three Degrees of Road Rash Severity and How to Identify Yours
Medical professionals classify road rash using the same system as burns because the tissue damage closely resembles thermal injury. Accurate self-assessment determines whether you need immediate emergency care or can manage recovery at home.
First-Degree Road Rash (Superficial)
Only the epidermis is affected. The wound appears red and raw, similar to a bad sunburn or rug burn. You'll feel stinging pain and see some weeping of clear fluid, but no significant bleeding. The skin surface remains intact enough that you can see it trying to regenerate.
Touch the area gently—if you can see skin texture and the wound blanches white when pressed, you're likely dealing with first-degree damage. These injuries hurt disproportionately to their severity because nerve endings remain intact and exposed.
Second-Degree Road Rash (Partial Thickness)
The dermis is compromised. You'll see a mix of red, raw tissue and white or yellow areas where deeper skin layers show through. Bleeding ranges from oozing to moderate, and blisters often form at the wound edges. The texture looks uneven—some areas appear scraped down to a shiny, moist surface while others show ragged skin flaps.
Pain intensifies with second-degree injuries, but here's a concerning paradox: if a section feels numb, that indicates nerve damage and suggests the wound is deeper than it first appears. Swelling around the wound margin is common and expected.
Third-Degree Road Rash (Full Thickness)
All skin layers are destroyed, exposing subcutaneous fat (appears yellow and lumpy), muscle (dark red and fibrous), or bone (white and hard). Paradoxically, these wounds may hurt less than second-degree injuries because nerve endings have been completely destroyed. You might see a leathery, charred appearance from friction heat.
Third-degree road rash requires immediate surgical intervention. The body cannot regenerate skin across these defects—they need grafting, flap procedures, or at minimum, specialized wound care to prevent life-threatening infection.
| Degree of Severity | Skin Layers Affected | Visual Symptoms | Healing Time | Scarring Risk | Professional Treatment Needed |
| First-Degree | Epidermis only | Red, raw, similar to sunburn; minimal bleeding | 5-10 days | Minimal; usually fades completely | No (unless covering large body area) |
| Second-Degree | Epidermis + partial dermis | Mixed red/white tissue; blisters; moderate bleeding; uneven texture | 2-6 weeks | Moderate; depends on care quality and location | Yes—for proper cleaning and infection prevention |
| Third-Degree | Full thickness (all layers) | Exposed fat, muscle, or bone; leathery or charred areas; numbness | 2-6 months (often requires grafting) | High; permanent scarring expected | Absolutely—emergency surgical consultation required |
This road rash severity motorcycle crash guide helps with initial assessment, but photograph your wounds daily. Injuries that look second-degree on day one may reveal deeper damage as dead tissue sloughs off over 48-72 hours.
Immediate Treatment Steps at the Accident Scene
The first 30 minutes after impact set the trajectory for your entire recovery. Adrenaline masks pain and clouds judgment, so follow this protocol even if you feel "fine."
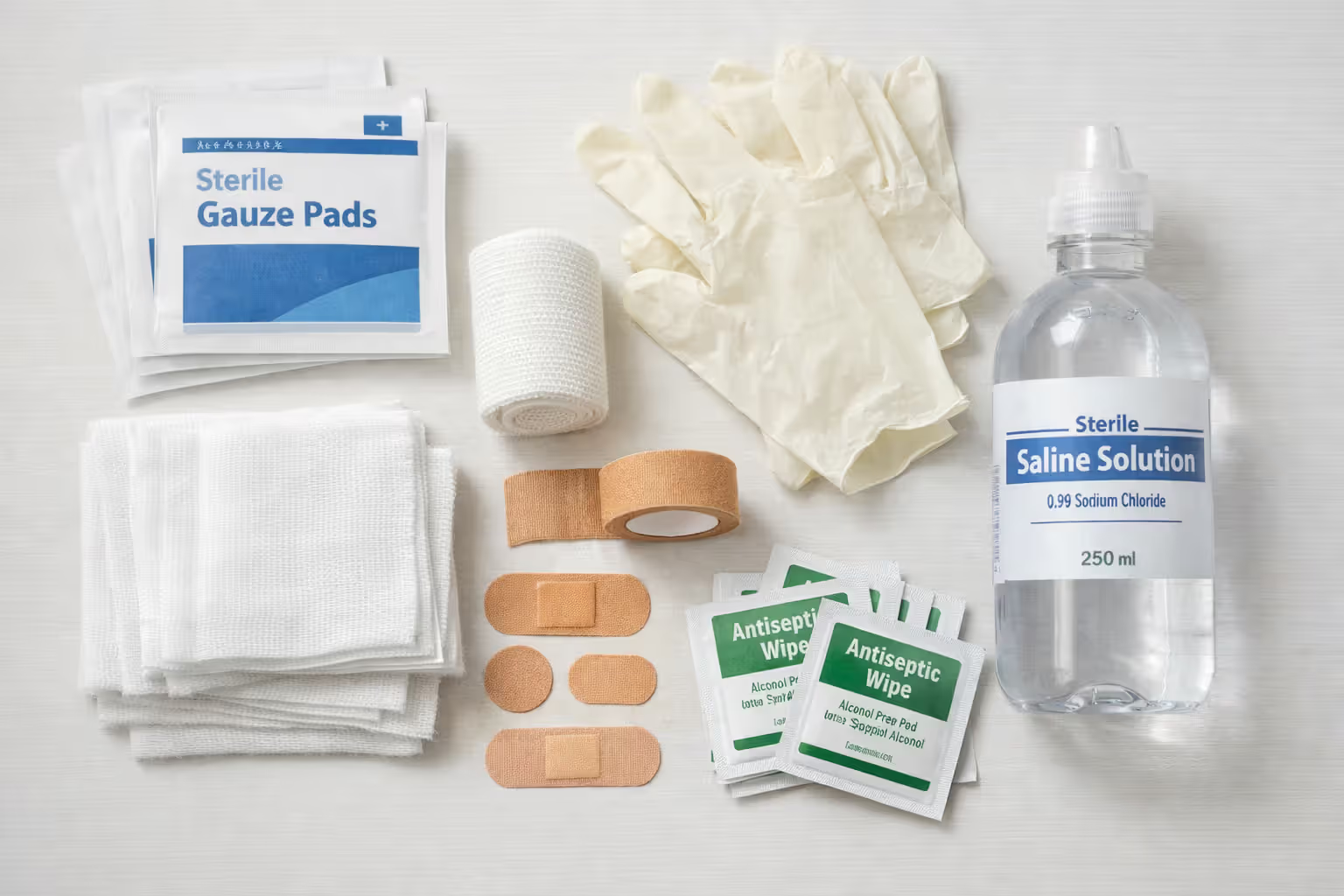
Stop any active bleeding first. Apply direct pressure with the cleanest available material—a shirt, bandana, or bystander's jacket. Don't waste time searching for sterile supplies. Bleeding from road rash rarely threatens life, but it obscures your ability to assess wound depth.
Do not attempt debris removal beyond loose surface material. Embedded gravel and asphalt require professional irrigation and debridement. Picking at embedded debris causes additional tissue damage and drives contaminants deeper. If you can brush it away without resistance, remove it. If it requires pulling or digging, leave it alone.
Cover the wound loosely. Exposed road rash collects more contamination every second it remains open. Use any clean, dry cloth as a temporary barrier. Avoid applying ointments, creams, or home remedies at this stage—they complicate subsequent medical cleaning.
Assess for shock and other injuries. Road rash hurts enough to distract you from a fractured wrist or internal bleeding. Before focusing entirely on skin damage, verify you can move all limbs, take deep breaths without sharp pain, and maintain clear thinking.
Call for professional help if: the wound is larger than your palm, you see fat or bone, bleeding doesn't slow after five minutes of pressure, you lost consciousness during the crash, or you're alone and feeling lightheaded. This road rash treatment motorcycle accident guide assumes you can think clearly—if you can't, you need an ambulance, not self-care.
One critical mistake: riders sometimes pour water bottles over road rash at the scene, thinking they're cleaning it. Unsterile water introduces new bacteria. Unless you have genuine sterile saline, leave wound irrigation to medical professionals.
Author: Ryan Whitlock;
Source: spy-delhi.com
Medical Treatment Protocol for Motorcycle Road Rash
Emergency Room vs. Urgent Care: Where to Go
Emergency departments handle third-degree injuries, wounds covering more than 10% of body surface area, road rash on the face or genitals, or cases where you have other injuries (suspected fractures, head trauma, chest pain). They have immediate surgical consultation available and can perform complex debridement under sedation.
Urgent care centers can manage most first- and second-degree road rash if the wounds are relatively small and you're otherwise stable. They'll clean, debride, dress, and prescribe antibiotics if needed. Wait times are shorter and costs run 40-60% less than ER visits.
For borderline cases, call ahead and describe your injury. Most urgent care facilities will tell you honestly if you need a higher level of care.
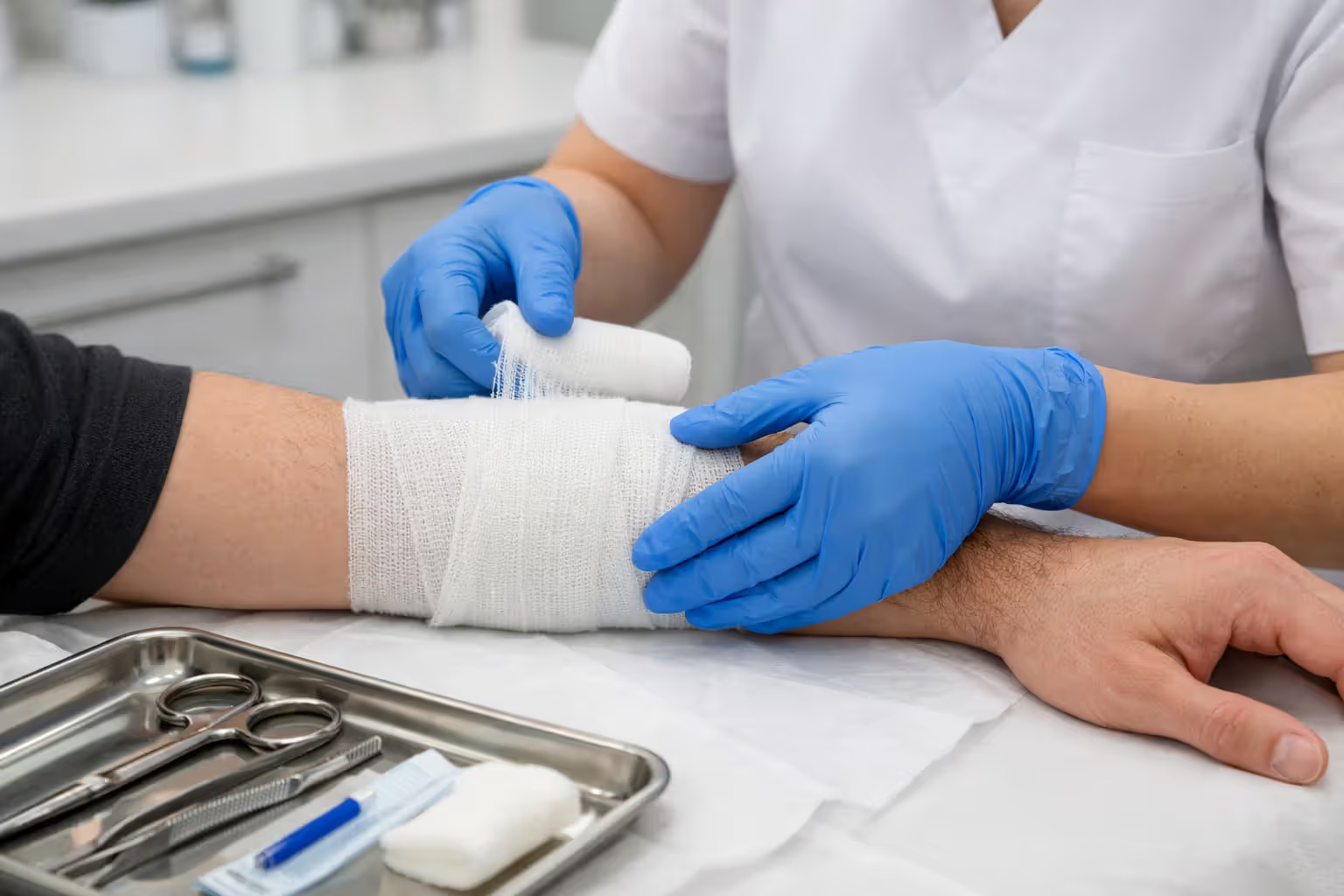
Wound Cleaning and Debridement Procedures
Proper cleaning is excruciating but non-negotiable. Medical staff will irrigate your wound with pressurized sterile saline—often liters of it—to flush out embedded debris. The pressure required to dislodge asphalt particles causes intense pain even through local anesthesia.
Debridement follows irrigation. Using sterile instruments, providers remove dead tissue, loose skin flaps, and any remaining foreign material. This road rash injury motorcycle accident guide emphasizes a hard truth: inadequate debridement is the number one cause of delayed healing and infection. Some providers rush this step. If you sense they're being superficial, request more thorough cleaning or seek a second opinion.
The single biggest mistake I see with motorcycle road rash is inadequate initial debridement. Riders tolerate maybe 60% of the cleaning they actually need, then wonder why they develop cellulitis five days later. If you can still see dirt or embedded debris after cleaning, the job isn't finished—period. I'd rather have a patient angry at me for being thorough than readmit them for IV antibiotics or surgical debridement of an infected wound
— Dr. Michael Chen
For extensive injuries, debridement may happen in an operating room under general anesthesia or conscious sedation. This allows surgeons to work methodically without causing unbearable pain and enables them to assess for deeper damage like tendon or nerve involvement.
Infection Prevention and Antibiotics
Not every road rash requires antibiotics, but most second-degree and all third-degree injuries warrant prophylactic coverage. Providers typically prescribe cephalexin or doxycycline for 7-10 days, targeting the skin bacteria most likely to colonize open wounds.
Tetanus status matters. If your last booster was more than five years ago, you'll receive one. The dirty, contaminated nature of road rash makes tetanus prophylaxis essential.
Severe cases—particularly those with delayed treatment, heavy contamination, or compromised immune systems—may require admission for IV antibiotics and serial wound checks. Don't refuse hospitalization if it's recommended. Necrotizing fasciitis (flesh-eating bacteria) is rare but documented in contaminated road rash cases.
Author: Ryan Whitlock;
Source: spy-delhi.com
Home Care and Recovery Timeline by Severity Level
First-degree road rash typically crusts over within 48 hours. Keep the area clean with gentle soap and water once daily. Apply a thin layer of petroleum jelly or antibiotic ointment, then cover with a non-stick pad and secure with breathable tape. Change dressings once daily. Most superficial injuries heal completely in 7-10 days.
Second-degree wounds follow a more complex timeline. Days 1-3 involve heavy drainage—clear to slightly bloody fluid is normal. Change dressings twice daily during this phase. By day 4-7, drainage decreases and you'll see pink granulation tissue (new tissue growth) forming at the wound base. This is healthy. Continue moist wound healing with petroleum-based products and non-stick dressings.
Weeks 2-3 bring epithelialization—new skin cells migrate across the wound surface, appearing as a thin, shiny layer advancing from the edges inward. Protect this fragile new skin obsessively. A single scrape or infection can destroy weeks of progress. By week 4-6, the wound should be fully closed but remains red, sensitive, and vulnerable to sun damage.
Third-degree injuries require professional wound care throughout healing. Expect 2-3 visits weekly initially, tapering to weekly checks. If you received skin grafts, the donor site (where they harvested healthy skin) often hurts worse than the original injury and follows its own 3-4 week healing timeline.
This road rash recovery motorcycle accident guide emphasizes one universal rule: maintain moist wound healing. Wounds heal 40% faster and with less scarring when kept moist versus allowing them to dry and scab. Use petroleum jelly, hydrogel sheets, or specialized wound dressings—never let road rash air dry.
Five Critical Mistakes That Delay Road Rash Healing
Mistake #1: Using hydrogen peroxide or alcohol. Both kill bacteria but also destroy the healthy cells trying to repair your wound. They delay healing by days to weeks. Stick with soap and water or sterile saline.
Mistake #2: Changing dressings too infrequently. Saturated dressings become bacterial breeding grounds. If your bandage feels wet or smells off, change it immediately regardless of your schedule. During heavy drainage phases, twice-daily changes are minimum.
Mistake #3: Ignoring early infection signs. Increased pain after day 3-4, expanding redness beyond the wound margin, warmth spreading outward, fever above 100.4°F, or pus with a foul odor all indicate infection. Waiting "to see if it gets better" allows infections to advance from superficial to deep tissue involvement. Call your provider at the first sign.
Mistake #4: Sun exposure on healing or healed wounds. UV radiation causes hyperpigmentation in healing skin that can be permanent. For six months after wound closure, keep the area covered or use SPF 50+ sunscreen religiously. Many riders skip this step and end up with dark scarring that otherwise would have faded.
Mistake #5: Returning to activity before wounds are fully matured. A closed wound isn't a healed wound. New skin remains fragile for 6-8 weeks after closure. Returning to riding, gym workouts, or manual labor too early causes wound breakdown—you'll literally split the new skin open and restart the healing timeline from zero.

Author: Ryan Whitlock;
Source: spy-delhi.com
Frequently Asked Questions About Motorcycle Accident Road Rash
Moving Forward After Road Rash
Road rash from motorcycle accidents tests patience more than almost any other injury. Broken bones heal on a predictable timeline; road rash healing varies wildly based on wound care quality, your overall health, and sometimes just luck. The difference between a wound that heals cleanly in three weeks versus one that festers for months often comes down to decisions made in the first 72 hours.
Prioritize thorough professional cleaning over pain avoidance. Follow wound care instructions exactly, even when it feels excessive. Watch for infection signs obsessively. Protect healing and healed skin from sun damage for months. These basics aren't glamorous, but they work.
Most riders eventually return to the activities they love, though many invest in better protective gear afterward. Road rash teaches respect for physics in ways that no safety course can match. Your skin regenerates remarkably well when given proper support—trust the process, follow medical guidance, and give your body the time it needs to rebuild what the pavement took away.
Related Stories

Read more

Read more

The content on this website is provided for general informational and educational purposes only. It is intended to offer insights and guidance on motorcycle accident insurance claims, settlement processes, liability issues, coverage limits, medical compensation, and related insurance matters, and should not be considered legal or financial advice.
All information, articles, and materials presented on this website are for general informational purposes only. Insurance policies, liability standards, settlement practices, and state regulations may vary by jurisdiction and insurer. The outcome of a motorcycle accident claim depends on the specific facts of the accident, available evidence, policy language, and applicable law.
This website is not responsible for any errors or omissions in the content, or for actions taken based on the information provided. Users are strongly encouraged to consult with a qualified attorney or licensed insurance professional regarding their specific motorcycle accident claim before making decisions about settlements, negotiations, or coverage disputes.




