
Crashed motorcycle lying on asphalt road with emergency ambulance lights in background
Motorcycle Accident Spinal Injury Guide to Treatment, Recovery, and Claims
Here's something that'll stop you cold: motorcycles make up less than 3% of vehicles on American roads, yet they're involved in roughly 5% of all spinal cord injuries. Those numbers tell you everything about the risks riders face every time they swing a leg over the seat.
When a motorcycle crashes, there's no metal cage protecting your spine. One moment you're riding. The next? Your entire future—your ability to walk, work, or even breathe on your own—hangs in the balance. Some riders heal completely. Others face permanent paralysis.
What happens in the first hour after a crash matters enormously. So does understanding which injuries you're dealing with, what treatments actually work, and how to protect yourself legally when medical bills start piling up into six or seven figures. Let's cut through the confusion and look at what you're really facing after a motorcycle accident damages your spine.
How Motorcycle Crashes Cause Spinal Cord Damage
Your spine holds 33 vertebrae stacked like blocks, cushioning the spinal cord inside. It evolved to handle normal movement—bending, twisting, the occasional stumble. But a motorcycle collision at 40 mph? That's not what nature had in mind.
Cars crumple by design. Their frames absorb crash energy through deformation zones. Airbags cushion your head and chest. Motorcycles offer none of this protection. When you hit something—or when something hits you—your body absorbs every ounce of force directly. Your spine takes the brunt.
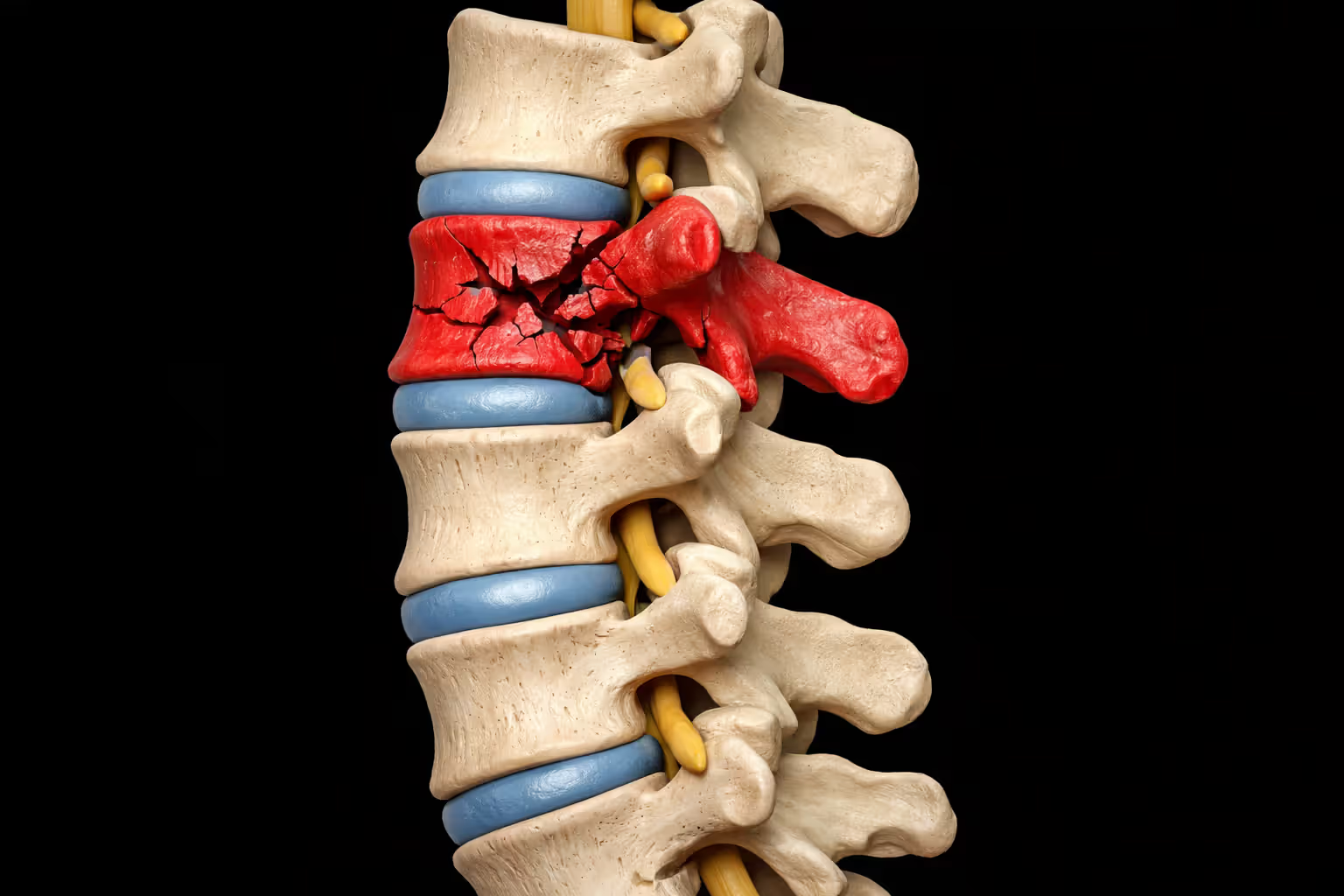
Three types of force destroy spinal integrity: compression (crushing vertebrae together), hyperextension (bending backward beyond normal range), and rotation (twisting motion that shears bone and ligament). Most serious crashes combine all three simultaneously.
Common Impact Scenarios That Lead to Back Injuries
A high-side crash flips you over the motorcycle like a catapult. You're airborne for a fraction of a second, body rotating uncontrollably. When you land—usually on your back or side—the thoracic vertebrae between your shoulder blades compress violently. T6 through T12 fractures are common here. The mid-back wasn't built for that kind of landing.
Head-on impacts whip your neck through extreme motion. Your torso keeps moving forward even as the bike stops or crumples. The cervical vertebrae in your neck hyperextend or flex past their limits. Sometimes the vertebrae break. Sometimes they don't need to—the spinal cord itself tears or bruises from the violent motion. Doctors call this SCIWORA: spinal cord injury without radiographic abnormality. X-rays look fine, but you're paralyzed anyway.
Getting rear-ended throws you into the handlebars or gas tank. Your lower back—specifically where L1 and L2 vertebrae sit—absorbs tremendous compression. This transition point between your flexible lumbar spine and rigid thoracic spine acts like a fault line. It's where burst fractures happen most often.
Even sliding out seems less dangerous until you factor in the tumbling. Your body becomes a spinning cylinder across pavement, generating torque that twists vertebrae out of alignment. Ligaments holding bones together can rupture without any fracture showing up on initial scans. Three weeks later, those unstable vertebrae shift and suddenly you've got paralysis that wasn't there at the accident scene.
Author: Hannah Pierce;
Source: spy-delhi.com
Why Motorcyclists Face Higher Spinal Trauma Risk
No protective shell exists around you. A car's steel frame distributes impact across engineered structures. You get leather and maybe some armor padding. Not the same thing.
Sitting upright means your spine runs vertical—a direct load path for forces during collision. Physics doesn't care about your riding skills. When vertical impact occurs, energy travels straight through each vertebra like stacking coins and smashing them from above.
Ejection introduces chaos. You might hit a guardrail edge-on, land on a curb corner, or slam into a vehicle after being thrown fifteen feet. Each scenario applies force from different angles. Your spine can't defend against impacts from multiple directions happening within seconds.
Speed multiplies everything. At 60 mph, your body carries massive kinetic energy that must dissipate instantly during a crash. Bones crack. Ligaments tear. The spinal cord—floating inside the vertebral column—slams against bone or stretches beyond what neural tissue can survive.
Types of Spinal Injuries From Motorcycle Accidents
Not every spinal injury causes paralysis, but all demand immediate medical evaluation. What matters most? Which structures got damaged and whether the spinal cord itself was compromised.
| Injury Classification | Location | Key Symptoms | Chance of Paralysis | Healing Duration |
| Compression Fracture | Mid to lower back (T1-T12, L1-L5) | Extreme back pain, can't move easily, sometimes numbness | Unlikely if cord stays intact | 2-3 months with brace |
| Burst Fracture | Lower back (L1-L2 usually) | Excruciating pain, weak legs, bladder or bowel problems | Moderate to significant | 3-6 months; surgery often needed |
| Chance Fracture (Flexion-Distraction) | Where thoracic meets lumbar | Stomach pain, tender back, nerve issues | Moderate possibility | 12-16 weeks; may require fusion |
| Fracture-Dislocation | Any level, cervical frequently | Complete or partial loss of movement below injury, no feeling | Very likely | 6+ months; permanent damage typical |
| Cord Contusion | Neck region (C1-C7) | Muscle weakness, strange sensations, can't breathe well if high up | Significant risk | Unpredictable; recovery may continue 12-18 months |
| Herniated Disc | Neck or lower back | Pain shooting down limbs, numbness, weak muscles | Minimal | 6-12 weeks usually; surgery sometimes |
Incomplete injuries—where some nerve signals still get through—give you better odds than complete injuries where absolutely nothing works below the damage site. Still, even incomplete injuries often leave you with permanent limitations you'll manage for life.
Central cord syndrome typically follows cervical hyperextension. Arms lose function more than legs. You might walk but can't button your shirt or hold a fork steadily. Brown-Séquard syndrome happens when fracture fragments or penetrating objects damage one side of the cord. You get weakness on one side of your body, sensation loss on the other side. It's weird and disorienting.
Immediate Steps After a Motorcycle Crash With Suspected Spinal Trauma
The first minutes after impact determine whether a survivable injury becomes catastrophic. Moving someone incorrectly can convert a stable fracture into complete paralysis. This isn't theoretical—it happens regularly at accident scenes.
Warning Signs That Require Emergency Response
Serious neck or back pain following any collision should trigger immediate immobilization. Yes, pain alone doesn't confirm spinal injury. But you don't gamble with these stakes. Call 911. Tell them explicitly you suspect spine damage.
Numbness or tingling anywhere below the injury—fingers, legs, feet, anywhere—indicates possible cord involvement. Might feel like your foot "fell asleep" or like pins and needles in your hands. Even if it goes away within minutes, damage may have occurred. Don't assume you're fine.
Weakness in your extremities, even subtle stuff like reduced grip strength or wobbly legs, suggests neurological compromise. Don't try walking it off. Don't test whether you can stand. Stay still.
Losing bladder or bowel control points to severe cord damage affecting autonomic functions. This symptom rarely appears without other obvious problems, but it represents an absolute medical emergency.
Trouble breathing or feeling like you can't take a full breath may indicate high cervical injury affecting nerves that control your diaphragm. Injuries at C3-C5 can cause respiratory failure. You need ventilator support immediately.
What NOT to Do at the Accident Scene

Author: Hannah Pierce;
Source: spy-delhi.com
Never yank off a helmet if you suspect spine injury unless you absolutely must perform CPR. Helmet removal requires two trained people using specific techniques to stabilize head and neck. Well-meaning bystanders who pull off helmets often convert non-displaced fractures into devastating cord injuries. Leave the helmet alone.
Don't let the injured rider stand up, sit upright, or move "to get comfortable." Maintain whatever position they landed in until EMS arrives with proper immobilization equipment. Face-down and breathing okay? Leave them face-down.
Don't offer food, water, or pain medication. Emergency surgery might be necessary within hours. Anything in the stomach increases anesthesia complications. Pain medication also masks symptoms doctors desperately need to assess accurately.
Don't wait to "see if it gets better" before calling for help. Spinal cord injuries have narrow intervention windows. Swelling and inflammation worsen over hours. Early treatment with anti-inflammatory protocols may limit secondary damage—but only if you get medical attention immediately.
Treatment Options and Recovery Timelines for Motorcycle-Related Spinal Injuries
Treatment paths split dramatically based on injury type, where it happened, and whether the cord sustained damage. Stable fractures without nerve problems follow completely different protocols than unstable injuries with cord compression.
Surgical vs. Non-Surgical Interventions
Conservative treatment works for compression fractures and certain burst fractures where the spinal canal isn't compromised. A rigid brace locks your spine in place for two to three months while bone knits back together. You can walk around, but you can't bend, twist, or lift anything. Physical therapy starts after initial healing restores strength and flexibility.
This approach sidesteps surgical risks but demands strict compliance. Taking off the brace too early or resuming normal activities prematurely can shift fractures that were stable. Then you've got delayed cord injury weeks after the accident—something that should've healed causes paralysis because you couldn't follow restrictions.
Surgery becomes necessary when fractures are unstable, bone fragments compress the cord, or vertebrae dislocate. Decompression surgery removes bone or disc material pressing on neural tissue. Fusion procedures install metal rods, screws, and bone grafts to permanently stabilize vertebrae. That spinal segment won't move again.
Surgery typically happens within 24-72 hours when cord compression exists. Earlier decompression might improve neurological outcomes, though evidence remains debated among surgeons. The procedure itself carries risks: infection, hardware loosening or breaking, adjacent segment degeneration, and rarely, worsened neurological deficits.
Recovering from spinal fusion takes three to six months before normal activities resume. Heavy lifting and high-impact sports may be permanently restricted. The hardware typically stays in your body for life unless it causes pain or complications requiring removal.
Rehabilitation Phases and What to Expect
Acute rehabilitation starts in the hospital within days of surgery or injury. Physical therapists check strength, sensation, and what you can move. For cord injury patients, occupational therapists evaluate hand function and teach adaptive techniques for daily tasks like dressing or eating.
First phase focuses on preventing complications: pressure sores from lying still too long, blood clots, pneumonia from shallow breathing, and muscle contractures that freeze joints in painful positions. You learn positioning strategies, skin inspection routines, and respiratory exercises.
Active rehabilitation begins once bone healing allows weight-bearing. Patients with incomplete cord injuries work on walking patterns, balance exercises, and coordination drills. Those with complete injuries learn wheelchair maneuvering, transfer techniques, and adaptive equipment operation.
Outpatient therapy keeps going for months or years afterward. Neurological recovery from cord damage follows no predictable timeline. Most improvement happens within six months, with diminishing gains after that. Still, some patients experience meaningful changes up to two years post-injury.

Author: Hannah Pierce;
Source: spy-delhi.com
Newer interventions like functional electrical stimulation, body-weight-supported treadmill training, and robotic-assisted therapy show promise for improving outcomes. They're not available everywhere. Often you'll pay out-of-pocket or travel to specialized centers—sometimes across multiple states.
Paralysis Risk and Long-Term Complications
Complete spinal cord injuries above C4 require ventilator support just to breathe. Injuries at C5-C6 preserve your diaphragm but paralyze trunk and leg muscles, severely limiting independence. Thoracic injuries cause paraplegia—legs don't work but arms remain functional.
The level and completeness of the initial injury largely determine long-term outcomes, but aggressive early intervention and comprehensive rehabilitation can maximize whatever recovery potential exists. We've seen patients with initially complete injuries regain some function, though predicting who will improve remains challenging
— Dr. Michael Fehlings
Beyond paralysis itself, long-term complications include chronic neuropathic pain affecting up to 80% of spinal cord injury patients. This burning, electric, stabbing pain originates from damaged nerves. Standard painkillers barely touch it. Medications like gabapentin or pregabalin provide partial relief for some people—but many patients never find adequate pain control.
Autonomic dysreflexia threatens anyone with injuries above T6. It's a life-threatening condition where blood pressure spikes dangerously in response to stimuli below the injury level—full bladder, ingrown toenail, tight pants. Without recognition and immediate treatment, it causes strokes or seizures.
Bone density below the injury level plummets, dramatically increasing fracture risk. Heterotopic ossification—abnormal bone growing in soft tissues around joints—can lock up range of motion and complicate rehabilitation efforts.
Bowel and bladder dysfunction require management programs involving scheduled catheterization, digital stimulation, or surgical interventions like suprapubic catheters. These routines consume hours daily. Urinary tract infections become a constant threat.
Sexual function changes after spinal cord injury, though many patients retain capacity for sexual activity and reproduction with modifications. Male fertility often decreases. Women typically maintain fertility but face pregnancy complications requiring specialized obstetric care throughout gestation.
Financial and Legal Considerations After a Spinal Injury Motorcycle Accident
The economic devastation of motorcycle-related spinal injuries extends decades beyond initial hospitalization. Understanding costs and legal options becomes critical for securing necessary care and compensation.
Average Medical Costs by Injury Severity
First-year expenses for high tetraplegia (C1-C4 injuries) average $1.1 million. Over a lifetime? We're talking $5 million-plus for a 25-year-old. Low tetraplegia (C5-C8) runs approximately $770,000 initially, ballooning to $3.7 million lifetime.
Paraplegia costs about $520,000 in year one, with lifetime expenditures around $2.4 million. These calculations factor in hospital stays, surgical procedures, rehabilitation programs, durable medical equipment, home renovations for accessibility, and attendant care services.
Incomplete motor functional injuries at any level require roughly $350,000 first-year costs and $1.6 million over your lifetime. These estimates assume typical complications—pressure ulcers, urinary tract infections, respiratory issues requiring periodic hospitalization.
Annual expenses after the first year range from $42,000 for incomplete injuries to $185,000 for high tetraplegia. These ongoing costs cover medications, medical supplies, personal care attendants, equipment maintenance, physician visits, and emergency care for complications.
Insurance rarely covers these needs adequately. Even comprehensive health insurance caps certain services, excludes experimental treatments, and limits durable medical equipment budgets. Medicare doesn't cover 24-hour attendant care. Medicaid requires spending down essentially all assets to qualify—goodbye savings, goodbye home equity.

Author: Hannah Pierce;
Source: spy-delhi.com
Compensation Claims and Statute of Limitations
If another party caused the accident—distracted driver, dangerous road defect, vehicle malfunction—personal injury claims can recover damages. Compensation categories include medical costs (past and future), lost wages, diminished earning capacity, physical pain and emotional suffering, and loss of consortium for spouses.
Statute of limitations varies by state. Typically you've got one to six years from the accident date to file suit. Miss this deadline? You're permanently barred from legal action. Some states pause the clock during periods of incapacity, but don't assume this protection applies without consulting an attorney.
Determining liability proves crucial. Pure comparative negligence states let you recover damages even if you were partially at fault—your compensation just gets reduced by your percentage of responsibility. Modified comparative negligence states bar recovery if you're 50% or 51% at fault (depending on state). Contributory negligence states (only a few still use this harsh standard) deny any recovery if you bear even 1% fault.
Insurance policy limits often fall catastrophically short of actual damages. The at-fault driver's $100,000 bodily injury coverage won't scratch the surface of $2 million lifetime costs. Underinsured motorist coverage on your own policy can fill gaps—but many riders carry minimum coverage to reduce premiums, leaving themselves exposed.
Structured settlements provide periodic payments rather than lump sums. They ensure long-term financial security but limit flexibility if your needs change. Lump sums offer control but risk depletion through poor investment decisions or unexpected expenses that blow through your cushion.
Third-party claims against helmet manufacturers (defects that contributed to injury), motorcycle manufacturers (design flaws that increased crash severity), or government entities (dangerous road conditions that caused the crash) may supplement driver liability claims. These cases demand expert testimony and extensive documentation—they're expensive to pursue and difficult to win.
Frequently Asked Questions About Motorcycle Accident Spinal Injuries
Moving Forward After a Motorcycle Accident Spinal Injury
Recovery from spinal injuries sustained in motorcycle accidents demands resilience, patience, and comprehensive support networks. Medical teams provide treatment protocols, but outcomes depend equally on your rehabilitation commitment, family support, and access to financial resources.
Document everything starting at the accident scene: medical records, itemized expenses, missed work days, and detailed notes about how injuries affect daily activities. This documentation becomes essential for insurance claims and potential litigation. Consult a personal injury attorney experienced specifically in catastrophic injury cases before accepting any settlement offers—initial offers almost never reflect true long-term costs insurers know you'll face.
Connect with spinal cord injury support groups and peer mentors who've already navigated similar challenges. Their practical advice about equipment selection, accessible housing modifications, employment accommodations, and emotional coping strategies often proves more valuable than clinical information from medical professionals.
Spinal injuries fundamentally alter life trajectories, no question. But they don't eliminate possibilities or meaning. Adaptive sports programs, modified career paths, and assistive technology enable many patients to rebuild satisfying lives around new limitations. Focus on achievable goals within your current capabilities rather than constantly mourning lost abilities. Some riders eventually return to motorcycling using adaptive equipment and modified bikes. Others discover new passions that never would've developed otherwise.
The road ahead stretches long and challenging after motorcycle accidents damage your spine. But understanding medical realities clearly, protecting your legal rights aggressively, and accessing appropriate resources consistently improves the journey. Whether you're facing months of recovery or permanent life changes, informed decisions and persistent self-advocacy make the difference between merely surviving day-to-day and genuinely living beyond the injury.
Related Stories

Read more

Read more

The content on this website is provided for general informational and educational purposes only. It is intended to offer insights and guidance on motorcycle accident insurance claims, settlement processes, liability issues, coverage limits, medical compensation, and related insurance matters, and should not be considered legal or financial advice.
All information, articles, and materials presented on this website are for general informational purposes only. Insurance policies, liability standards, settlement practices, and state regulations may vary by jurisdiction and insurer. The outcome of a motorcycle accident claim depends on the specific facts of the accident, available evidence, policy language, and applicable law.
This website is not responsible for any errors or omissions in the content, or for actions taken based on the information provided. Users are strongly encouraged to consult with a qualified attorney or licensed insurance professional regarding their specific motorcycle accident claim before making decisions about settlements, negotiations, or coverage disputes.




